March 31, 2025, 2:35 pm | Read time: 10 minutes
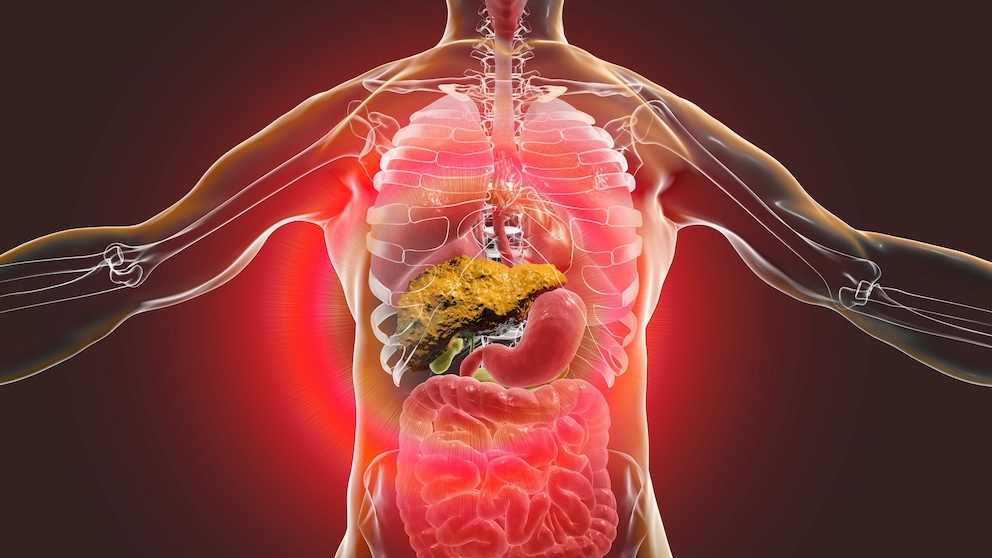
Many people only go to the doctor when they feel pain. One organ that has no nerves and, therefore, cannot cause pain is the liver. The organ plays a key role in our metabolism and, as a “detoxification organ,” converts toxic substances into harmless substances that we excrete again. Chronic liver disease, infections, or overworking the liver can lead to cirrhosis. If the disease remains undetected and untreated for too long, it can be fatal for those affected.
The incidence of liver cirrhosis is very high, at around 250 cases per 100,000 people. Men are affected twice as often as women. The disease refers to the gradual scarring of liver tissue. Healthy liver tissue is gradually transformed into functionless connective tissue, i.e., scar tissue, which reduces the organ function of the liver. If liver cirrhosis remains undetected and untreated, the liver can fail completely in the final stage — which can lead to death. The tricky thing is that signs and symptoms of the disease only appear when the cirrhosis is already well advanced. Many people, therefore, do not realize for a long time that they have the disease, which means that cirrhosis of the liver cannot be treated at an early stage.
Overview
Symptoms of Liver Cirrhosis
Early Symptoms
Early symptoms of liver cirrhosis are often very general and varied, which means that other reasons for the symptoms often come to mind. Signs of early liver cirrhosis can include:
- feeling tired and weak
- loss of appetite
- unwanted weight loss
- nausea and vomiting
- discomfort in the upper right side of the abdomen
There are also symptoms caused by a possible underlying disease that has caused liver cirrhosis. These include, for example, the metabolic disease Wilson’s disease, which is inherited in an autosomal recessive manner and in which reduced copper excretion can lead to deposits in the liver and subsequently to liver cirrhosis. The copper deposits in other organs can also trigger symptoms such as memory, speech, and muscle disorders.1
Symptoms in the Later Stages
In the later stages of liver cirrhosis, the liver may enlarge or shrink. If there is an enlarged liver and spleen, which can also enlarge due to liver cirrhosis, this is referred to as hepatosplenomegaly. Cirrhosis of the liver can also be noticeable on the skin, known as liver skin signs. These characteristic changes to the skin can be
- yellow discoloration of the skin and eyes (icterus, also known as “jaundice”)
- star-shaped formation of new blood vessels, particularly localized on the face and décolleté (so-called spider naevi)
- increase in abdominal circumference, possibly with accumulation of abdominal fluid (ascites)
- increased vein pattern on the abdomen (so-called caput-medusae)
- redness on the palms of the hands and soles of the feet (palmar erythema)
- lacquer lips and lacquer tongue (smooth, red, dry lips and tongue)
- itching (pruritus)
The hormone balance is also disrupted by the damage to the liver, as sex hormones such as estrogen can no longer be broken down properly. In men, this can lead to loss of hair on the abdomen, but also to shrinking testicles, loss of libido, and impotence. In women, liver cirrhosis can lead to menstrual cycle disorders or missed periods.2
Possible Complications of Liver Cirrhosis
If the liver is too heavily scarred, at some point, it can no longer compensate for the loss of functional cells. The so-called decompensated liver cirrhosis then leads to various complications. Some of these can have life-threatening consequences.
Blood Congestion or Portal Vein Hypertension
Very severe scarring of the liver means that blood can no longer flow properly through the organ. As a result, the blood builds up, and high blood pressure develops in the portal vein, the large blood vessel in the abdomen that carries blood from the intestines and other digestive organs to the liver. This portal vein hypertension can cause blood to back up and the vessels to dilate, which can lead to the development of varicose veins in the stomach and especially in the esophagus (known as oesophageal varices). Burst esophageal varices can manifest as massive hematemesis and can quickly become life-threatening.
Portal vein hypertension can lead to the leakage of tissue fluid due to a backlog of blood, which in turn leads to the accumulation of this fluid in the free abdominal cavity. These so-called ascites cause the abdominal circumference to increase and bulge forward. If the fluid presses on the diaphragm, breathing problems can also occur.
Lack of Detoxification (hepatic encephalopathy)
If the damage to the liver is too advanced, it can no longer detoxify sufficiently, and toxins enter the brain. The complication of hepatic encephalopathy is a consequence of the increase in toxins in the blood, which then enter the brain and potentially disrupt brain metabolism. Signs of this can include sleep disorders, mood swings, tremors, loss of consciousness, severe cognitive impairment, and multiple neuropsychiatric abnormalities. However, this process may still be reversible with appropriate treatment.
Disruption of the Metabolism
The liver plays a key role in the body’s metabolism. Nutrients that are absorbed into the blood in the intestine enter the liver via the portal vein and are further utilized, converted, broken down, or stored there. Sugar is also stored in the liver in the form of glycogen and then released back into the blood as glucose when required. Proteins, which are important for blood clotting, are also produced in the liver.
If the liver can no longer fulfill these functions due to the breakdown of healthy liver cells, this can lead to metabolic disorders that manifest themselves as diabetes mellitus or blood clotting disorders.
Causes
Liver cirrhosis can have various causes. Among other things, it develops in the final stage of chronic liver disease, which can be caused by viral infections, liver-damaging influences over a long period of time, or autoimmune and metabolic diseases.
Alcohol Abuse
In Western industrialized countries, long-term alcohol abuse is responsible for more than half of all liver cirrhosis. As a metabolic and detoxification organ, the liver breaks down toxic alcohol. In the process, more toxins are produced in the liver cells, such as acetaldehyde. Such toxins promote abnormal fat storage in the liver, which can lead to a fatty liver.
If alcohol abuse continues over a long period of time, liver fibrosis develops, whereby the fatty liver cells are replaced by connective tissue, which then appears as liver fibrosis (i.e., scarring). If the fibrosis continues to develop unabated, it eventually leads to liver cirrhosis. The functional liver cells die, and the liver becomes completely scarred, which then manifests itself as shrinkage of the liver.
Fatty Liver
It does not necessarily take regular alcohol consumption to develop a fatty liver. In non-alcoholic fatty liver disease (NAFLD), excess fat is also stored in the liver. Non-alcoholic steatohepatitis (NASH) is the name given to the form of fatty liver that causes inflammation and damage to the liver, which can lead to liver fibrosis and, under certain circumstances, cirrhosis. This type of fatty liver is usually caused by a very unhealthy, sugary diet, diabetes, and morbid obesity.3
Liver Cirrhosis Due to Viral Hepatitis
Alongside alcohol abuse, chronic liver inflammation caused by hepatitis viruses of types B and C is the most common cause of cirrhosis of the liver worldwide. Chronic inflammation can then lead to scarring and damage to the liver cells, causing them to eventually die.
Other Possible Causes
There are also other causes, such as
- autoimmune diseases of the liver and gallbladder, such as immune-related inflammation of the liver (autoimmune hepatitis) or inflammation of the bile ducts (primary biliary cirrhosis)
- metabolic diseases, such as Wilson’s disease or cystic fibrosis
- tropical diseases
- heart disease
- contact with toxic substances, e.g., chemicals such as arsenic
- medication and medication abuse
If none of the known causes of cirrhosis can be identified, it is referred to as cryptogenic cirrhosis of the liver.4
Diagnosis
If you recognize symptoms in yourself and suspect liver disease, the only thing that helps — as always — is to see a doctor. A detailed medical history, i.e., questioning about medical history and all medically relevant information, as well as a detailed physical examination, can provide information about possible causes and liver damage. Of course, if liver damage is suspected, further tests are required to determine whether the liver is damaged and to what extent. These include, among other things
- a complete blood count to determine deficiencies,
- liver enzymes, as an indication of damage to the liver cells,
- blood coagulation tests,
- test for albumin, a protein produced in the liver,
- liver function tests,
- alpha-fetoprotein, a liver cancer screening,
- upper endoscopy to look for varicose veins in the esophagus,
- ultrasound examinations of the liver,
- MRI and CT scans of the abdomen
- liver biopsy
If there is a suspicion that the liver damage has already caused brain damage, additional psychometric tests are carried out.
Stages of Liver Cirrhosis
In order to classify the stage of the disease, the symptoms of cirrhosis are assessed using the so-called Child-Pugh criteria.5 The score that results from the assessment gives the Child-Pugh score, which is divided into the following categories:
| Score | Stage | Liver function | 1-year survival rate |
|---|---|---|---|
| 5-6 Points | Child A | good liver function | ca. 100% |
| 7-9 Points | Child B | moderate liver function | ca. 85% |
| >10 Points | Child C | Low liver function | ca. 35% |
Depending on the stage, different measures must be taken. While life expectancy is still relatively high in the Child-Pugh A stage, the prognosis worsens as the Child-Pugh score increases and the disease progresses.
Treatment Options
The liver is very resilient and can regenerate damaged cells well. However, cirrhosis itself is irreversible, i.e., the scarred tissue cannot “recover.” Therapy can only treat previously damaged cells and thus halt or slow down the progression of cirrhosis.
The earlier cirrhosis of the liver is detected and treated, the better the prognosis. In order to halt the progression of liver cirrhosis, the underlying cause or disease must first be clarified and treated. If alcohol addiction is the cause of the liver damage, treatment for the addiction is necessary, while medications may be used to manage chronic hepatitis.
Depending on the cause and stage, your doctor will recommend appropriate treatment measures. In principle, further unnecessary stress on the liver caused by alcohol or liver-damaging drugs should be avoided, thereby causing further damage. However, this measure should also only be taken in consultation with a doctor. Both discontinuing medication on one’s own and abruptly stopping alcohol can be life-threatening for individuals with alcoholism or those dependent on medication.
Treatment of the Complications of Liver Cirrhosis
The stage of the disease and the associated complications also play a role in the treatment method. Individual complications, such as ascites, varicose vein bleeding in the esophagus, infections, or brain dysfunction, often need to be treated separately. If liver function becomes increasingly impaired due to the progression of cirrhosis and there is a risk of complete liver failure, a liver transplant may be the only option.
Lifestyle Factors and Diet
Many patients with advanced liver cirrhosis are malnourished. As with so many diseases, it is advisable to eat a balanced and healthy diet — in consultation with the doctor treating you — to counteract deficiency symptoms. Fatty acids and sugar should be avoided and attention should be paid to a high protein intake. Foods such as shellfish, fish, and meat, which may harbor viruses or bacteria, should be excluded from the diet. Alcohol should also be avoided completely.6
In large quantities Not just alcohol! 6 things that are harmful to the liver
Cervical Carcinoma Causes, Symptoms and Treatment of Cervical Cancer
Ask the expert Can I combine aspirin, paracetamol, and ibuprofen?
Conclusion
Depending on which complications occur, those affected must also pay attention to the salt content and the amount they drink. Either way, individual coordination is required, which should only be carried out by a doctor.7
The earlier cirrhosis of the liver is detected and treated, the better the prognosis. Regular check-ups at the doctor’s can detect possible liver disease at an early stage. Causes can be treated and lifestyle factors that damage the liver can be changed at an early stage. To prevent liver damage, it is important to avoid unnecessary strain on your liver, such as from alcohol abuse, a diet high in fats and sugars, or excessive medication use. Of course, everything should be done in consultation with a doctor.