February 8, 2025, 9:53 pm | Read time: 8 minutes
Cervical cancer is one of the tenth most common forms of cancer in women in Germany. FITBOOK author Julia Kuntz explains what causes this disease, how it develops, and what the symptoms and treatments can be.
Cervical cancer is one of the most common cancers in women worldwide. In Germany alone, more than 4,000 women are diagnosed with the disease every year.1 The good news is that thanks to modern medicine and targeted preventive measures such as the HPV vaccination, the disease is often preventable or at least easily treatable at an early stage. Despite its seriousness, many women still know very little about the symptoms and risk factors of the disease. FITBOOK asked expert Dr. Sabrina Bergstein, a specialist in gynecology and obstetrics in Düsseldorf, how you can recognize warning signs and actively prevent the disease as well as the treatment of cervical cancer.
Overview
- What Is Cervical Cancer?
- HPV (Human Papillomaviruses) – The Main Cause of Cervical Cancer
- Other Risk Factors for the Development of Cervical Cancer
- Prevention
- Main Types of Cervical Cancer
- Symptoms of Cervical Cancer
- Treatment of Cervical Cancer
- Treatability and Life Expectancy
- Progression If Not Treated
- Wanting to Have Children After the Treatment of Cervical Cancer?
- Is Cervical Cancer Inherited?
- Conclusion: Focus on Prevention and Vaccination
- Sources
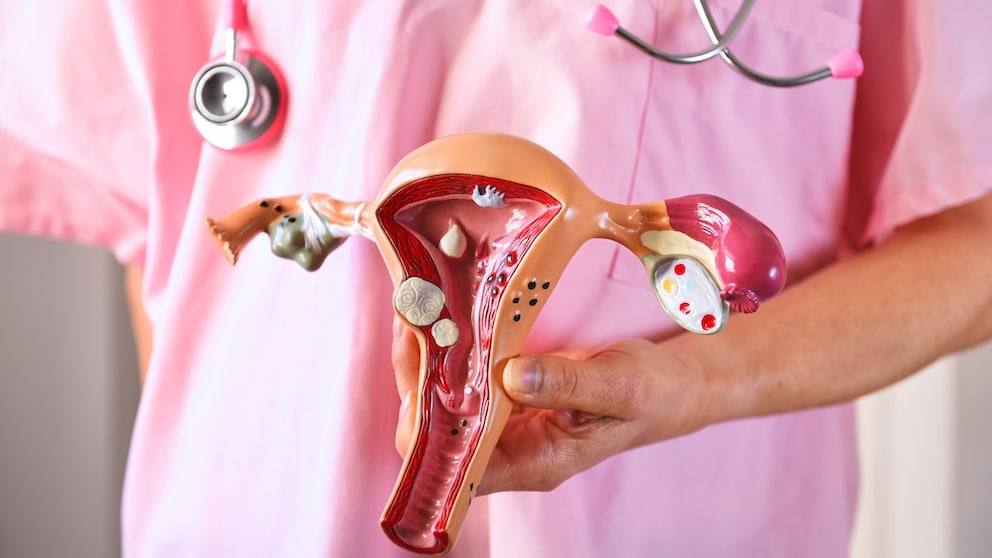
What Is Cervical Cancer?
Cervical cancer, also known as cervical carcinoma, occurs when the cells in the area of the cervix, i.e., the lower part of the uterus, multiply uncontrollably and form tumors.2 These can grow, invade surrounding tissue, and spread (metastasize) to other organs via blood or lymph vessels. The lymph nodes in the pelvic area are often affected first before the cancer spreads to more distant organs such as the lungs, liver, or bones. In contrast, there are also benign growths, such as polyps or harmless cysts, that grow non-invasively and do not form metastases.
HPV (Human Papillomaviruses) – The Main Cause of Cervical Cancer
What is HPV?
“The main cause of cervical cancer is considered to be persistent infection with high-risk HPV types,” says Dr. Bergstein. “HPV comprises a group of over 200 virus types, of which around 12 high-risk HPV types are considered to be reliably carcinogenic. These are of particular relevance as they can cause the cell changes that can lead to cancer, especially cervical cancer.”
Transmission of HPV
HPV is mainly transmitted through direct contact with the skin or mucous membranes, especially during sexual intercourse. The viruses are very contagious, and an infection can be barely noticeable, even without visible symptoms.3
Prevention
As part of cancer prevention, women should have a regular Pap test carried out by their gynecologist from the age of 20.4 From the age of 35, a combined Pap and HPV test is recommended every three years. The HPV vaccination is also a good preventive measure and is sometimes the best. It should be given between the ages of 9 and 14, before the first infection and ideally before the first sexual contact.
What do the HPV levels on a Pap Test Mean?
Five Pap stages assess the condition of the cells in the cervix:5
- Pap I: Normal cell image, no abnormalities.
- Pap II: Slight cell changes, often inflammation-related, usually harmless.
- Pap III: Unclear cell changes that should be investigated further.
- Pap IV: Severe cell changes, suspected precancerous stages.
- Pap V: Cells with evidence of cervical cancer.
Men Are Also Affected
What many people don’t know is that men can also be infected with HPV. Certain types of HPV can lead to genital warts or, in rare cases, to cancer in the genital area, anus or throat. HPV does not usually cause visible symptoms in men, but they can transmit the virus through sexual contact, including vaginal, anal, and oral intercourse. The HPV vaccination is, therefore, recommended not only for girls but also for boys from the age of 9.
The Course of an HPV Infection
As HPV infections are often asymptomatic, prevention is crucial in order to detect possible cell changes at an early stage. The body heals most HPV infections on its own, but there is an increased risk of cancer in the case of prolonged infections with high-risk types.
Other Risk Factors for the Development of Cervical Cancer
In addition to HPV infection, there are other factors that can increase the risk of developing the disease. An early onset of sexual activity and multiple sexual partners increase the risk, as the probability of infection with HPV increases with the number of contacts. In addition, a weakened immune system, for example, due to HIV or immunosuppressive medication, can significantly impair the body’s ability to fight an HPV infection. Smoking is also considered a risk factor, as nicotine damages the cells and weakens the immune system, which also makes it more difficult for cell changes to heal.
Prevention
Regular check-ups with a gynecologist can prevent up to 90% of cancer cases. They are the key to early detection and the avoidance of severe progression and complications. In addition to the HPV vaccination, regular exercise and a healthy lifestyle that strengthens the immune system and reduces the risk of infection are good preventive measures.6 Avoid nicotine and eat a balanced diet rich in vitamins and minerals. Always use condoms during sexual intercourse with different sexual partners to reduce the risk of contracting HPV or other sexually transmitted infections.
Main Types of Cervical Cancer
There are two main types of cervical cancer, which differ in their development and frequency. Squamous cell carcinomas develop in the outer layers of the cervix and account for around 70-80% of all cases.7 This form is the most common and is often due to infection with high-risk HPV types. Adenocarcinomas, on the other hand, develop in the glandular cells of the cervical canal and are less common but are often more aggressive. Both forms require early diagnosis and treatment.
Symptoms of Cervical Cancer
Most cases are diagnosed in women between the ages of 35 and 55. As the cancer develops slowly, it often takes years before it becomes noticeable. Also, the symptoms are often subtle, especially in the early stages, and are easily attributed to other causes. For this reason, early medical clarification is absolutely essential. If you experience the following symptoms, you should be alert and consult your gynecologist:
- Bleeding after sexual intercourse
- Spotting or discharge with an unpleasant odor
- Irregular bleeding between menstruation
- Pain in the pelvic area
Treatment of Cervical Cancer
Medical Therapy
“Treatment depends on the stage of the disease and the patient’s general state of health,” explains Dr. Bergstein. “In the early stages, when the cancer is limited to the cervix, minimally invasive procedures are usually sufficient. This primarily includes conization, in which a cone-shaped part of the cervix is removed with a scalpel or a snare. These methods make it possible to preserve the uterus and recover quickly. In advanced stages of the disease, when the cancer has spread to surrounding tissue, a combined treatment is required. This usually involves surgery to remove the uterus and possibly neighboring lymph nodes, followed by radiation and chemotherapy to destroy any remaining cancer cells and prevent recurrence as far as possible.”
What You Can Do Yourself
In addition to medical treatment, you can support your recovery and strengthen your immune system by adopting a healthy lifestyle with a balanced diet, regular exercise, and avoiding risk factors such as smoking. Close cooperation with the treatment team and regular follow-up examinations are also crucial for successful treatment.
Treatability and Life Expectancy
The chances of recovery depend heavily on the time of diagnosis. If the cancer is detected early, the cure rate is over 90%. Effective options for the treatment of cervical cancer are also available at later stages, although the course of the disease can become more complicated. Statistically, the 5-year survival rate is between 60% and 90%, depending on the stage.
Progression If Not Treated
If left untreated, cervical cancer progresses through several stages and can have serious consequences. In the early stages, the disease often remains asymptomatic, so that it initially goes unnoticed. Over time, the first symptoms may appear, such as unusual bleeding or pain in the lower abdomen. The tumor continues to grow and affects the surrounding tissue, such as the uterus, bladder, or bowel. Without treatment, the cancer can spread via lymph and blood vessels, leading to the formation of metastases in other organs such as the lungs, liver, or bones. In advanced stages, the disease often causes severe pain, organ failure, and considerable impairment of quality of life. Ultimately, untreated cervical cancer usually leads to death.
Wanting to Have Children After the Treatment of Cervical Cancer?
In the early stages, fertility-preserving treatment may be possible. Talk to your doctor about your plans early on to find the best options.
Is Cervical Cancer Inherited?
Cervical cancer is not usually genetic but is mostly caused by HPV infections. Nevertheless, genetic factors can influence the immune response.

Recognize Warning Signs These Skin Changes May Indicate Advanced Liver Cirrhosis
Study shows A severe coronavirus infection can possibly shrink cancer tumors
Developed by Stanford Researchers New Method to Increase the Effectiveness of the Flu Vaccine
Conclusion: Focus on Prevention and Vaccination
Cervical cancer is a serious but preventable disease. Through prevention, a healthy lifestyle, and, above all, the HPV vaccination, you can actively help protect yourself and your health. The HPV vaccination is usually covered by health insurance and is one of the most effective preventative measures. Studies show that the vaccination reduces the risk by up to 70%. The vaccination is considered safe and is recommended by the Standing Committee on Vaccination (STIKO) for all children and adolescents.